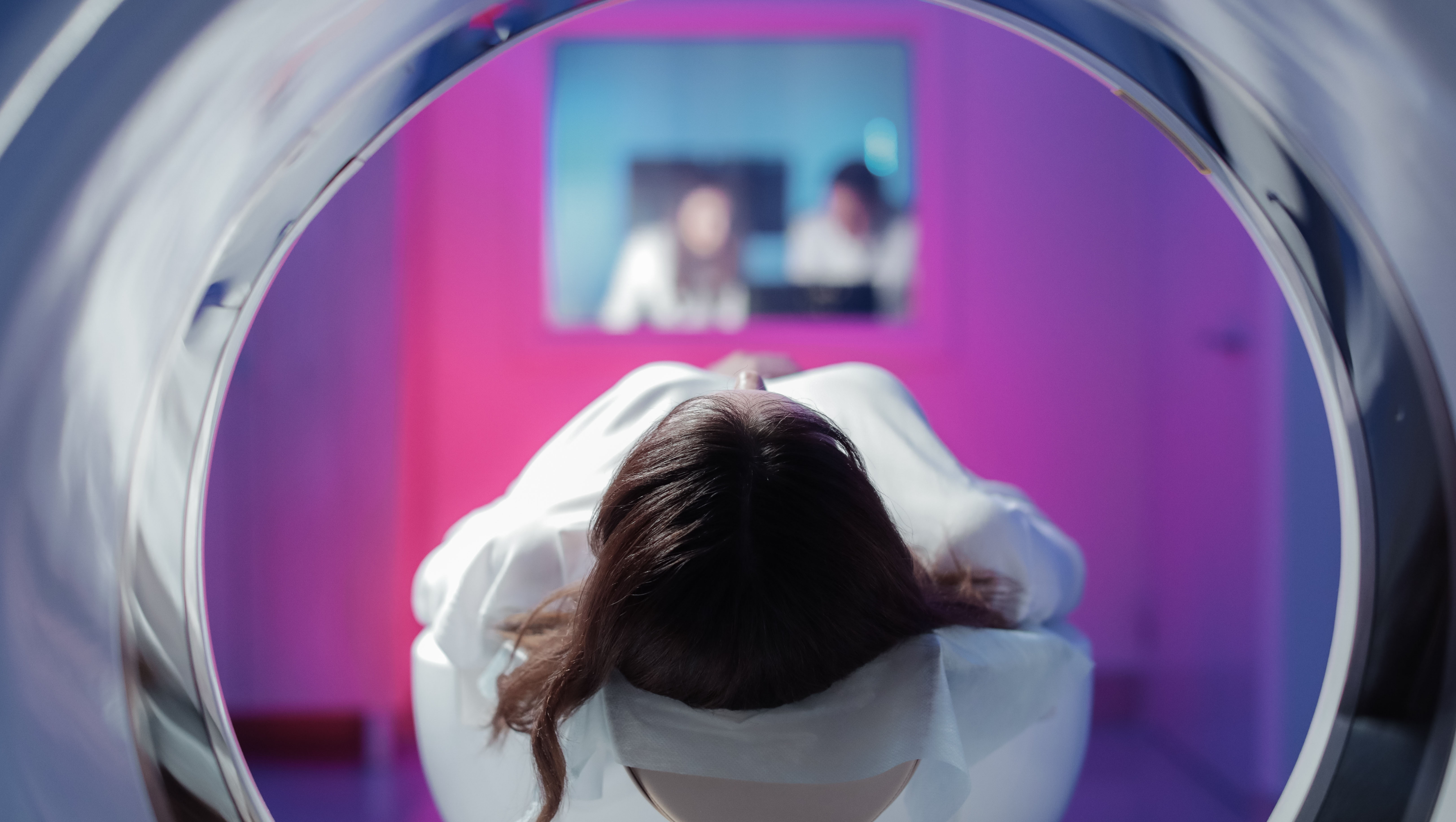
A new subsection of the CPT[i] code book has been established for reporting six new codes describing MR safety services, including implant or foreign body evaluation, safety consultation, electronics preparation, and implant positioning or immobilization. The new subsection is Magnetic Resonance (MR) Safety Implant/Foreign Body Procedures of the Radiology/Diagnostic Radiology (Diagnostic Imaging) and it contains the codes along with the guidelines for reporting them.
Categories:
radiology coding,
MRI,
radiology
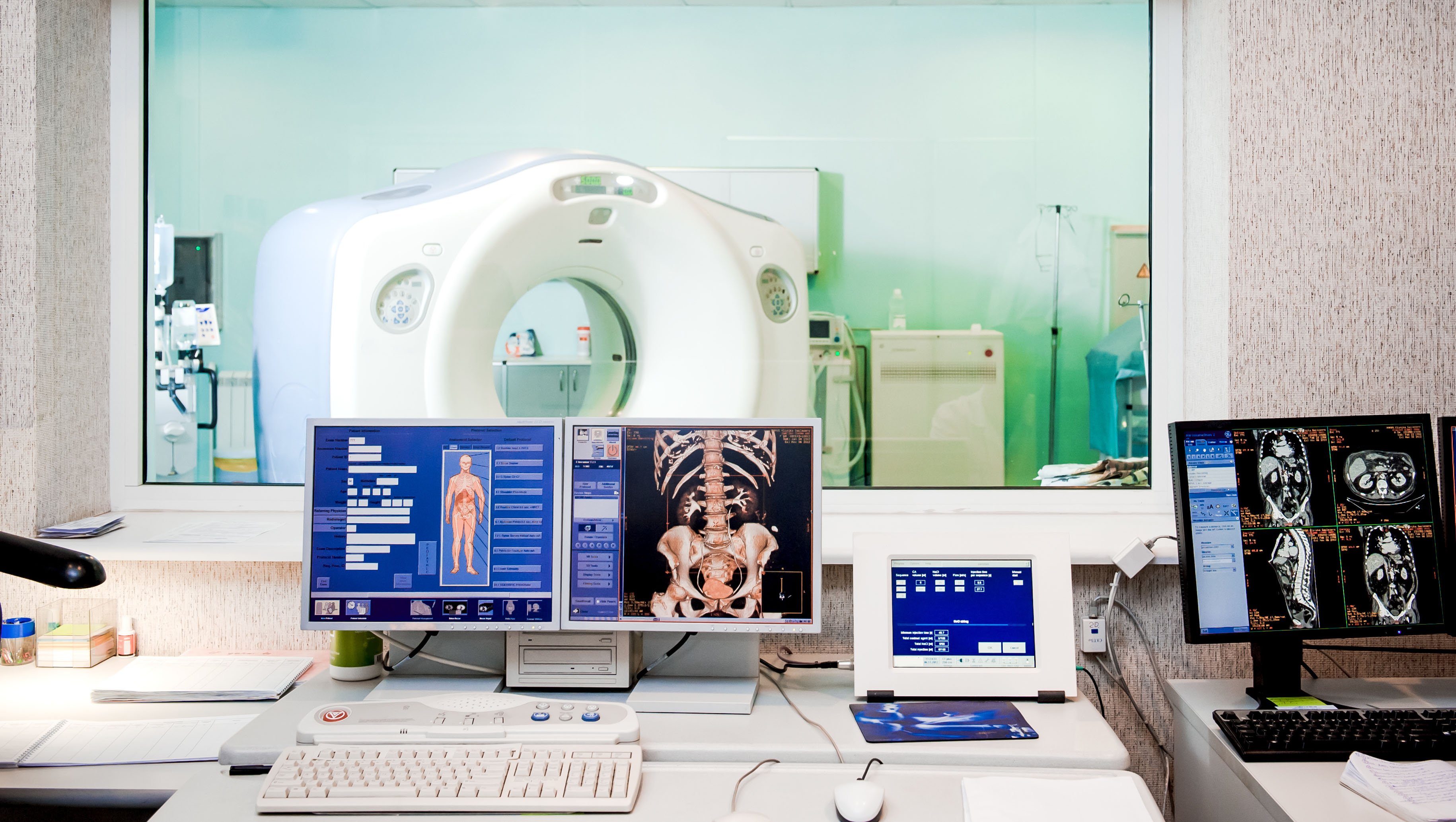
The Medicare Physician Fee Schedule (MPFS) for 2025 included coverage for screening CT Colonography (CTC), which had not previously been covered by Medicare. With the recent issuance of Change Request 13939 by the Centers for Medicare and Medicaid Services (CMS), all Medicare carriers now have the direction and authority to begin reimbursement for CTC.
Categories:
radiology,
CT Colonography
The Medicare reimbursement rates for 2025 remain unchanged as a result of the Continuing Resolution (CR) passed by Congress and signed on March 15. Thus, the downward spiral of Medicare reimbursement continues with physicians receiving nominally 2.83% less this year than in 2024. Radiology practices will see somewhat different results depending on their practice pattern, as we reported in our recent article analyzing the real impact of the Medicare Physician Fee Schedule (MPFS). We calculate that the Professional Component reimbursement would decrease 2.16%, while global reimbursement at an imaging center would decrease by 3.55%, both on a weighted-average basis.
Categories:
radiology reimbursement,
radiology,
continuing resolution
The 2025 conversion factor (CF) that sets the overall rate for the Medicare Physician Fee Schedule (MPFS) was adjusted downward by 2.83% from the 2024 rate, to $32.3465 per Relative Value Unit (RVU) vs. $33.2875 per RVU. Several bills are pending in Congress that would mitigate the scheduled reduction, at least on a temporary basis, or perhaps to make more permanent corrections to the Medicare pricing formula. However, as of this writing none are in active discussion.
Categories:
radiology reimbursement,
MPFS,
radiology,
Medicare Physician Fee Schedule
Radiology practices often participate in the Quality Payment Program (QPP) through the Merit-based Incentive Payment System (MIPS). Many aspects of the MIPS rules remain unchanged for 2025, including:
Categories:
radiology reimbursement,
MIPS,
Quality Payment Program,
MIPS participation,
QPP
The 2025 update to the Current Procedural Terminology[i] (CPT)® has 270 new codes, 38 revised codes, and 112 deleted codes. In addition, the ICD-10-CM[ii] update has over 300 revisions, additions and deletions. Although relatively few of these changes will impact radiology practices, it’s essential to know what they are and adjust your practice systems accordingly.
Categories:
interventional radiology,
CPT codes,
diagnostic radiology,
E&M,
evaluation and management
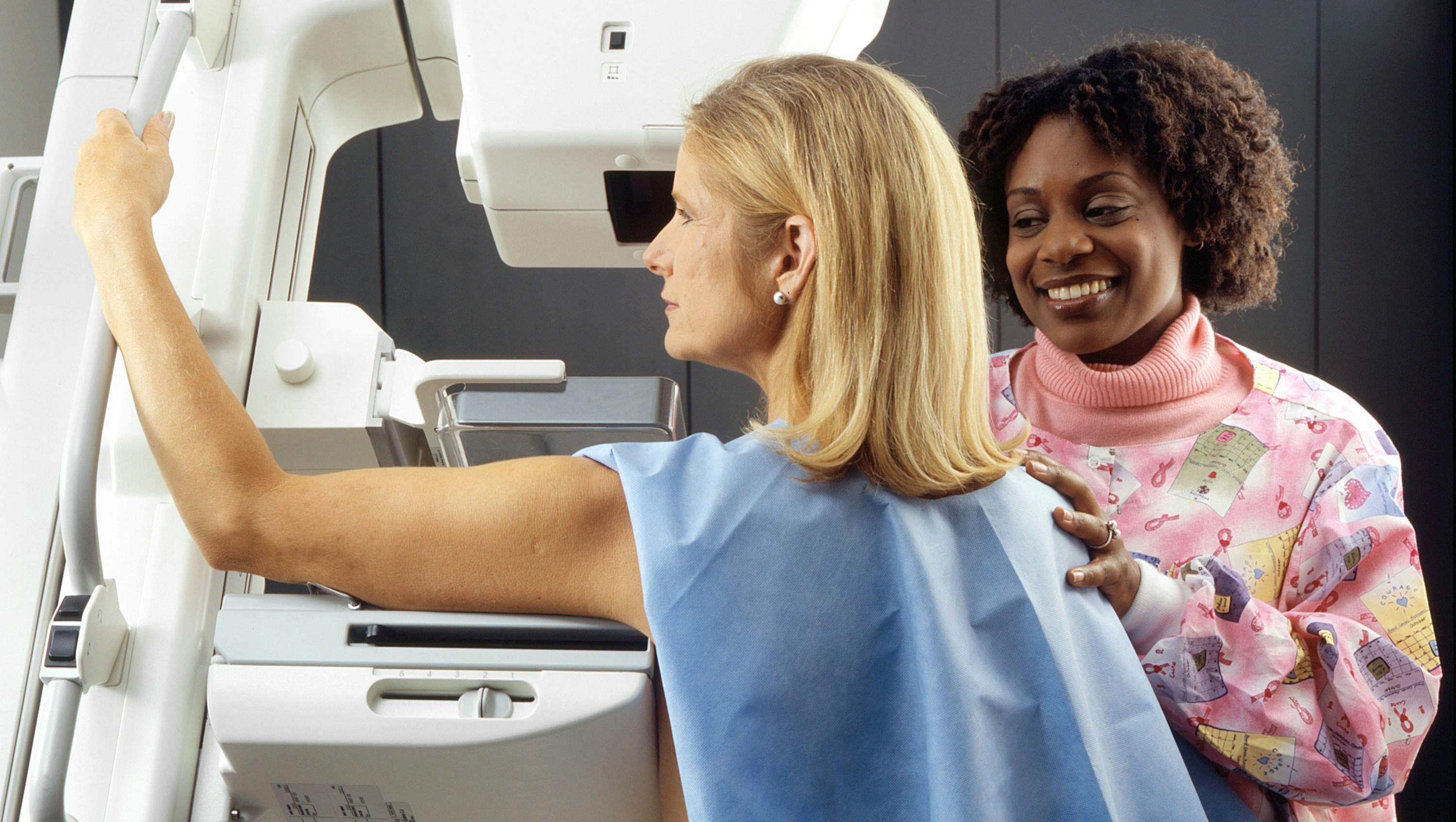
Mammography remains one of the most critical areas of radiology practice, and one that is facing changes in reporting requirements and reimbursement policy. Even with additional mammography reporting requirements placed on radiology practices, the reimbursement value of mammography services has not changed to reflect the extra work. However, changes to screening policy could provide increased mammography volume.
Categories:
mammography
Every business in the country has to evaluate its obligation to comply with the Corporate Transparency Act (CTA) by December 31, 2024. The CTA was enacted as part of the Federal Anti-Money Laundering Act of 2020, and the regulations became effective on January 1, 2024. Many practices may already have complied with the law by either submitting the required information or by determining that they are exempt from filing. Failure to comply may invoke civil penalties of $591 per day along with criminal penalties of two years in prison and a $10,000 fine.
Categories:
radiology
In April, 2020, the Federal Medical Assistance Percentage (FMAP) was increased so that states would receive extra funding for their Medicaid programs in support of the COVID-19 public health emergency. In exchange, the states promised to pause Medicaid eligibility checks so that more people would be able to continue to receive Medicaid benefits to get through the pandemic.
Categories:
radiology,
medicaid
Absent any last-minute Congressional action, physicians will suffer a 2.83% fee schedule reduction for 2025. This is slightly more of a cut than had been predicted in the Medicare Physician Fee Schedule (MPFS) Proposed Rule that was issued in July. As we reported in our analysis of the Proposed Rule, this reduction in payments continues a trend that has seen the Medicare fee schedule reduced by nearly 10% over the past 10 years. The Medicare cuts for 2025 are just the latest example.
Categories:
medicare,
medicare reimbursement,
MPFS,
Quality Payment Program,
Medicare Physician Fee Schedule








.jpg)