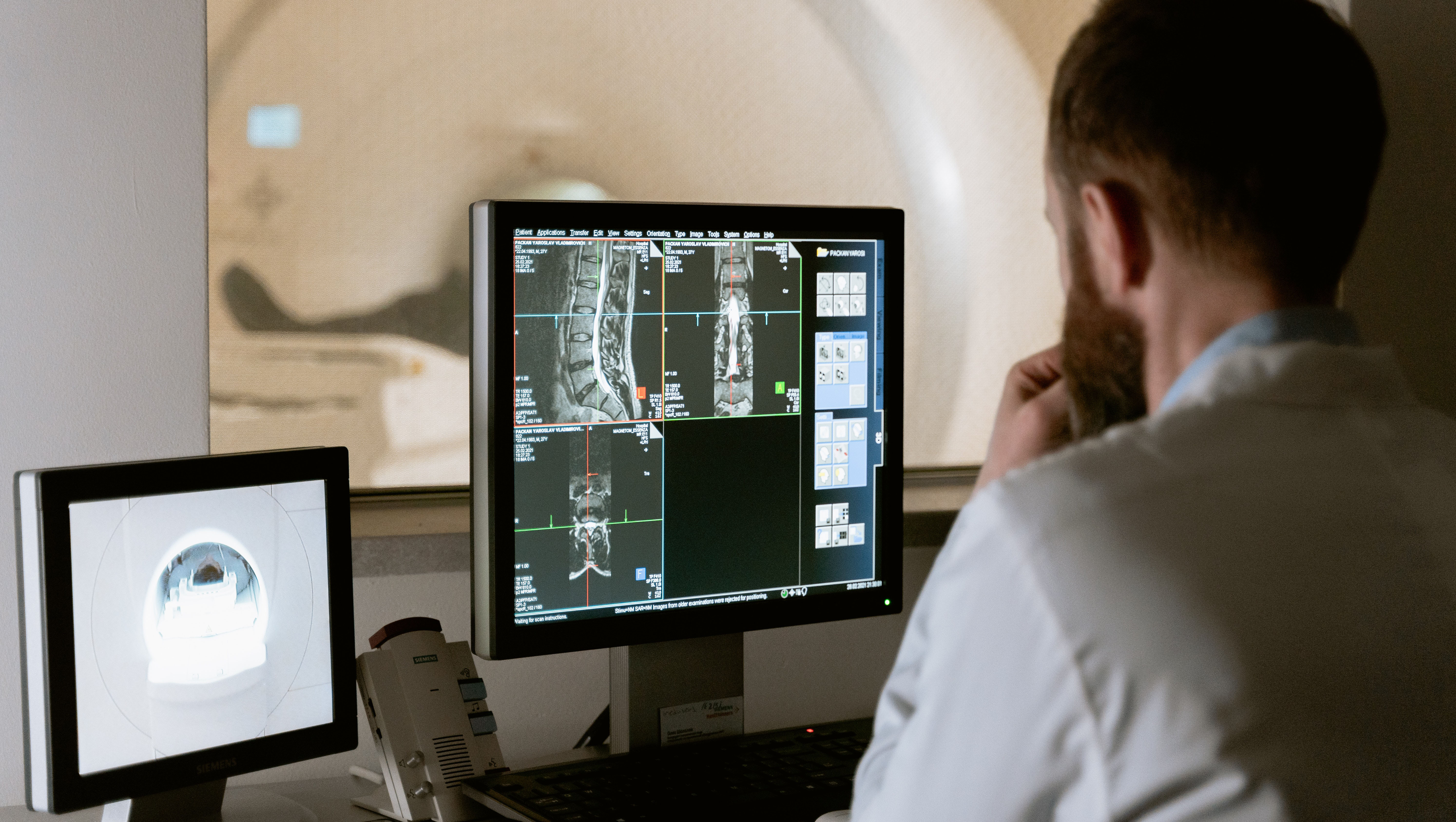
Radiology practices often participate in the Quality Payment Program (QPP) through the Merit-based Incentive Payment System (MIPS). Many aspects of the MIPS rules remain unchanged for 2025, including:
Categories:
radiology reimbursement,
MIPS,
Quality Payment Program,
MIPS participation,
QPP
Practices that reported under the Merit-based Incentive Payment System (MIPS) of the Quality Payment Program (QPP) for 2023 can now get their performance score and find out how it will impact their Medicare reimbursement in 2025. The first step is to sign in to the QPP website to get your own practice’s results and review it for any discrepancies. The Centers for Medicare and Medicaid Services (CMS) has released the 2023 MIPS Performance Feedback FAQ’s as a guide to learning more about your practice’s performance.
Categories:
MIPS,
Quality Payment Program,
MIPS participation,
radiology,
QPP
The rules and requirements for success in the Medicare Quality Payment Program (QPP) are ever-changing, and it seems like each year brings a new challenge for practices to avoid a payment penalty or, hopefully, to earn a payment bonus. Most recently, CMS announced that the 2023 data submission deadline would be extended until April 15, 2024, due to the cyberattack at Change Healthcare in February, and that practices affected by the cyberattack could apply for an Extreme and Uncontrollable Circumstances (EUC) Exception. The EUC exception allows the applicant to request reweighting of any or all of the performance categories under the Merit-Based Incentive Payment System (MIPS).
Categories:
MIPS,
MIPS participation,
radiology,
QPP
The Centers for Medicare and Medicaid Services (CMS) announced its Medicare Physician Fee Schedule (MPFS) Final Rule for 2024, including provisions for both Medicare reimbursement and the Quality Payment Program (QPP).
Categories:
interventional radiology,
cms,
MPFS,
radiology,
QPP,
diagnostic radiology
For many radiology practices, the idea of a positive payment adjustment for participation in the Medicare Quality Payment Program (QPP) has been lost. Several factors have combined over the past few years to change the goal for radiology practices – it is now ‘penalty avoidance’ rather than a reward for reporting quality metrics. As we outlined in our recent review of the Medicare 2024 Physician Fee Schedule Proposed Rule, the QPP requirements for successful participation are going to become even stricter.
Categories:
MIPS,
Quality Payment Program,
MIPS participation,
radiology,
QPP,
quality measures
The Centers for Medicare and Medicaid Services (CMS) announced its proposed Medicare Physician Fee Schedule (MPFS) rules for 2024, including provisions for the Quality Payment Program (QPP). While not a done deal until the final rule is issued toward the end of the year, the Proposed Rule gives an indication of where CMS is headed with regard to payment policy. In recent history, even the Final Rule isn’t final because Congress has had to intervene to stave off significant reimbursement reductions. Here are the highlights of the 2024 Proposed Rule.
Categories:
medicare,
medicare reimbursement,
radiology,
QPP,
Medicare Physician Fee Schedule
Today's Quality Payment Program (QPP) began in 2006 as the Physician Quality Reporting Initiative (PQRI). It was a voluntary program that would earn participants a bonus payment of 2% of their prior-year Medicare reimbursements. Beginning with performance year 2013 (for payments in 2015) a penalty was imposed on those physicians who did not successfully report quality data. The 2016 performance year saw the initiation of the Value-Based Payment Modifier (VM) that allowed for upward, downward, or neutral payment adjustments in 2018 based on both the quality and cost of care delivery. In the first year the VM was applied, physicians with low cost and high quality earned an additional 9.78% over the basic Medicare fee schedule while the potential negative adjustment for not reporting, or not successfully reporting, was 6%. There was a lot of incentive to participate in the program at as high a level as possible!
Categories:
MIPS,
MIPS participation,
radiology,
QPP
The Centers for Medicare and Medicaid Services (CMS) press release announcing the Medicare Physician Fee Schedule (MPFS) Proposed Rule for 2023 highlights expanded access to behavioral health services, Accountable Care Organizations (ACO), cancer screening, and dental care. Of these areas, cancer screening could be important to radiology practices, but the news was not good – CMS declined to include CT colonography coverage while it expanded coverage for traditional colonoscopy. The MPFS regulates the Medicare fee schedule payment provisions as well as the Quality Payment Program (QPP).
Categories:
radiology reimbursement,
cms,
MPFS,
MIPS,
MIPS participation,
radiology,
QPP
Keeping abreast of the various healthcare rules and regulations from federal and state authorities can sometimes be overwhelming for a practice’s management. Here is a summary of some of the most important regulatory issues to be aware of for next year, along with a few payment policy decisions that are not governmental. The links will take you to our recent articles and other sources that probe each topic in more depth.
Categories:
cms,
MPFS,
low dose CT,
CPT codes,
radiology,
QPP,
surprise billing
The Quality Payment Program (QPP) continues to be modified due to the COVID-19 public health emergency. The Centers for Medicare and Medicaid Services (CMS) recently announced some leeway for clinicians affected by the pandemic in 2020 and 2021.
Categories:
radiology reimbursement,
cms,
QPP,
COVID-19