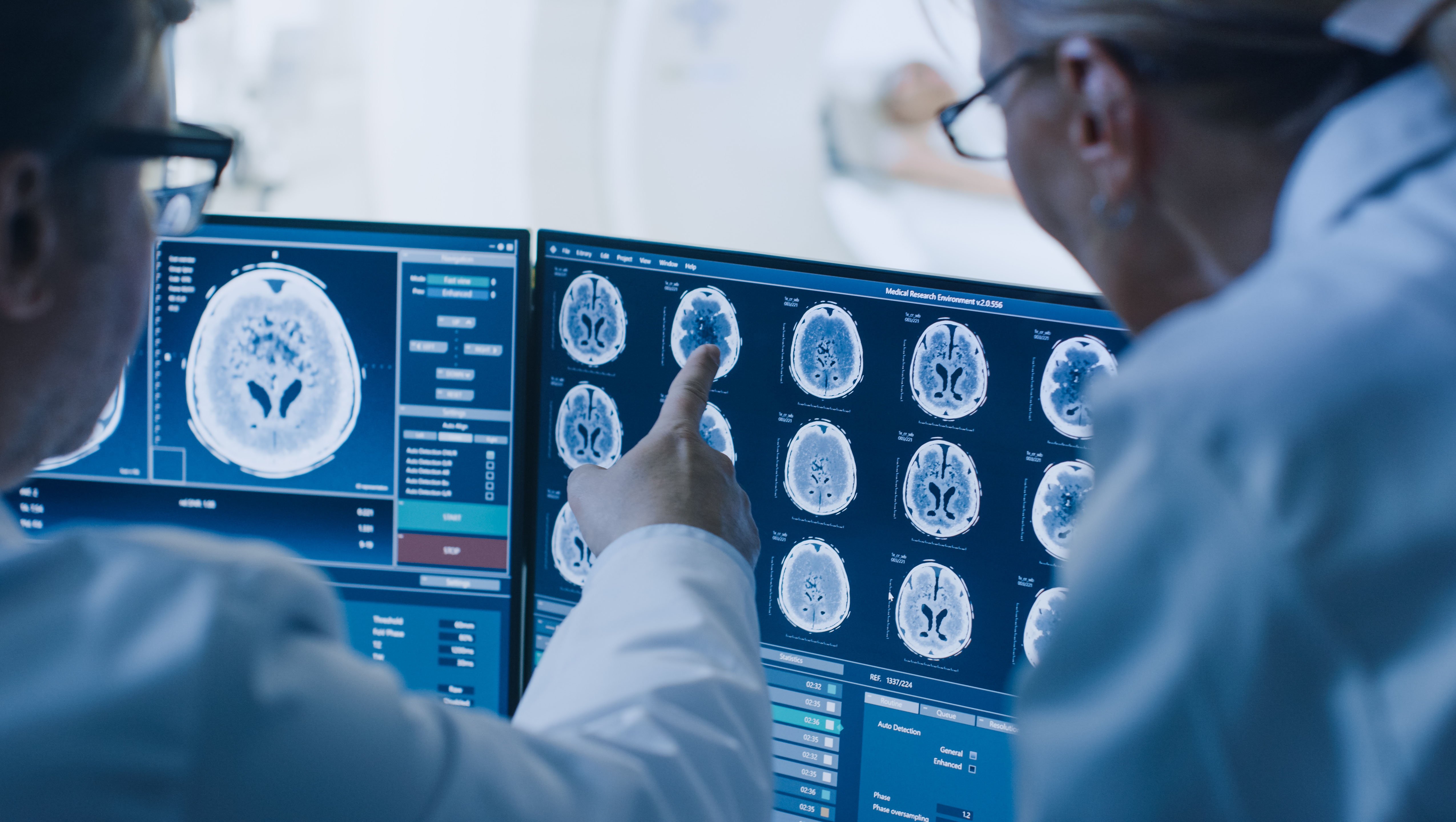
The annual update to the Current Procedural Terminology[1] (CPT)® for 2024 has 230 new codes, 70 revised codes, and 49 deleted codes. In addition, there are 395 new diagnosis codes contained in the ICD-10-CM[2] update, about one-third of them describing new ways to capture accidents and injuries. Although relatively few of these changes will impact radiology practices, it’s essential to know what they are and adjust your practice systems accordingly.
Coding Changes That Will Impact Diagnostic & Interventional Radiology Practices in 2024 on January 29, 2024
Categories: radiology coding, icd-10, interventional radiology, IR coding, CPT codes, diagnostic radiology
2024 Medicare Physician Fee Schedule Final Rule Includes Payment Reductions for Radiology on November 8, 2023
The Centers for Medicare and Medicaid Services (CMS) announced its Medicare Physician Fee Schedule (MPFS) Final Rule for 2024, including provisions for both Medicare reimbursement and the Quality Payment Program (QPP).
Categories: interventional radiology, cms, MPFS, radiology, QPP, diagnostic radiology
Coding Changes That Will Impact Radiology Practices In 2023 on January 23, 2023
Click here to read our 2024 code changes update article.
While only a few of the 225 new codes, 93 revised codes, and 75 deleted codes in Current Procedural Terminology[i] (CPT)® for 2023 will impact radiology practices, it’s essential to know what they are and adjust your practice systems accordingly.
Categories: radiology coding, interventional radiology, IR coding, CPT codes, diagnostic radiology, evaluation and management
Rural Care Settings Need More Radiology Expertise on December 8, 2022
Recently, a study by a joint task force of the American College of Radiology (ACR) and the Society of Interventional Radiology (SIR) pointed out the need for all diagnostic radiologists to have certain competencies in “Level 1” interventional procedures. Radiology Business reports that the aim of the task force was making recommendations for “broadening access to image-guided procedures for patient populations living in rural care settings or served by small IR practices.” According to the study abstract, “Radiology practices characterized as small and rural are challenged to recruit and retain interventional radiologists”, resulting in a failure to meet the needs of patients and others in these communities. Thus, having diagnostic radiologists with Level 1 competencies in small practice or rural health settings increases their ability to provide a wider range of needed services.
Categories: interventional radiology, radiology, rural health
Coding And Documentation For Arterial Embolization on August 29, 2022
Arterial catheter embolization is an interventional radiology procedure that requires detailed documentation of the steps performed by the physician to maximize coding and reimbursement. The procedure places medications, embolic agents, or a radiopharmaceutical into a blood vessel to prevent abnormal bleeding, close off vessels, eliminate abnormal connections between arteries and veins, or to treat aneurysms or tumors. Common embolization procedures include treatment of uterine fibroids or destruction of liver tumors using y-90 radioembolization.
Categories: radiology documentation, interventional radiology, IR coding
Mid-Year Radiology Coding Update and Other Reminders on July 29, 2022
Most updates to procedural and diagnosis coding become effective at the beginning of the year, but there are always a few mid-year changes that occur. In recent years, coding has changed to accommodate the COVID-19 public health emergency, and there are a few additions this year as well. Along with those, we’ll also add some reminders about topics that we’ve covered before.
Categories: radiology coding, interventional radiology, low dose CT, radiology, Provider Relief Fund, telehealth
Appropriate Use Criteria (AUC) Penalty Phase Set to Begin on April 29, 2022
Will the requirement to use Clinical Decision Support (CDS) finally become a reality? The current timetable for the penalty phase of the AUC/CDS rule calls for it to begin on the later of January 1, 2023, or the January 1 following the end of the COVID-19 public health emergency (PHE). The PHE has just been extended another 90 days into July 2022, with no end in sight although there are some indications that it could end this year. One source reports that the Administration will give 60 days’ notice before ending the PHE. With this uncertainty, it would be wise for practices to be ready just in case!
Categories: interventional radiology, clinical decision support, CDS, radiology, appropriate use criteria, AUC
Strengthening Congressional Support Addresses Medicare Interventional Radiology Cuts on February 25, 2022
Interventional radiology is among those specialties hit hard by the clinical labor practice expense cuts in the 2022 Medicare Physician Fee Schedule (MPFS). The proposed Physician Fee Schedule for 2022 contained an estimated 9% cut to interventional radiology (IR), due primarily to the revision of the practice expense component of the RVU calculation. The MPFS final rule brought the IR cut down to an estimated 5% after reconsideration of some of the methodology employed in calculating clinical labor costs. However, this is a blended figure that ignores the much larger effect on the global reimbursement for office procedures than on the professional component for hospital-based procedures.
Categories: interventional radiology, interventional radiology billing, Medicare Physician Fee Schedule
A radiology practice that includes interventional procedures has to be up to date on the use of documentation and coding techniques for Evaluation and Management (E&M) services. Since these CPT®[i] codes in the 99xxx range are less commonly utilized in many radiology practices, identifying circumstances where E&M services are billable, and then properly documenting and coding for them, will require a collaborative effort between interventional radiologists (IR) and their coding team.
Categories: interventional radiology, IR coding, interventional radiology billing, E&M, evaluation and management
Coding Changes That Will Impact Radiology Practices In 2021 on January 6, 2021
Click here to read our 2024 code changes update article.
The big news in Current Procedural Terminology[i] (CPT)® revisions for 2021 is the overhaul of the Evaluation and Management (E&M) section, reducing documentation requirements, and introducing new rules for determining the level of coding. These changes will affect interventional radiologists and radiation oncologists more than they will the day-to-day work of diagnostic radiologists. First, we will review the other non-E&M code changes affecting diagnostic and interventional radiology for 2021.
Categories: radiology coding, interventional radiology, IR coding, CPT codes, radiology, diagnostic radiology